University certificate
The world's largest faculty of veterinary medicine”
Introduction to the Program
Better trained veterinarians means longer life expectancy for animals. Don’t think twice and develop your skills in the field of Veterinary Cardiology with this complete Advanced master’s degree”
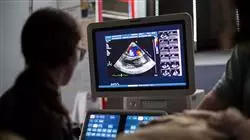
In recent years, considerable progress has been made in the area of Veterinary Cardiology , favored by the appearance of many new diagnostic and therapeutic techniques that have achieved successful results in the treatment of animals with heart disease.
Given these developments and the changing nature of the field, veterinary professionals must be in the habit of updating their knowledge in order to keep up with the applications of the most effective tools used in daily practice. That is the framework that structures this online Advanced master’s degree, complemented by the added benefit of all the latest developments in Veterinary Cardiology on the market today, both in small animals and larger species.
When it comes to larger species, further study is still needed in the field. For example, Cardiology in ruminants and swine has been limited for a long time due to the scarce literature available and diagnostic limitations, especially in advanced therapeutic procedures. Similarly, equidae are often affected by heart disease due to the overexertion required of them, especially horses participating in sports competitions. That is why it is necessary to have specialized veterinarians who are able to improve animal health and quality of life.
Furthermore, this specialization is aimed at professionals who normally have long working days, which prevents them from being able to continue specializing in traditional face-to-face classes, and who cannot find quality online programs adapted to their needs. Given this context of need, TECH presents this Advanced master’s degree in Veterinary Cardiology , which has come to revolutionize the world of veterinary specialization, both for its contents and for its teaching staff and innovative teaching methodology.
What’s more, as it is a 100% online specialization, students decide where and when to take on the course load. Without the restrictions of fixed timetables or having to move between classrooms, this course can be combined with work and family life.
A highly scientific program, supported by advanced technological development and the teaching experience of the best professionals”
This ##ESTUDIO## in Veterinary Cardiology contains the most complete and up-to-date scientific program on the market. The most important features include:
- The latest technology in e-learning software
- Intensely visual teaching system, supported by graphic and schematic contents that are easy to assimilate and understand
- The development of practical case studies presented by practicing experts
- State-of-the-art interactive video systems
- Teaching supported by telepractice
- Continuous updating and recycling systems
- Self-organized learning which makes the course completely compatible with other commitments
- Practical exercises for self-assessment and learning verification
- Support groups and educational synergies: questions to the expert, debates and knowledge forums
- Communication with the teacher and individual reflection work
- Content that is accessible from any fixed or portable device with an Internet connection
- Supplementary documentation databases are permanently available, even after the program
Advances in Veterinary Cardiology make it necessary for clinicians to constantly update their knowledge in order to know how to implement the latest techniques in their daily work”
Our teaching staff is made up of practicing professionals, ensuring that we offer the up-to-date information we intend to. A multidisciplinary staff of trained and experienced professionals from a variety of areas who will impart theoretical knowledge in an efficient manner, but above all, will contribute the practical knowledge derived from their experience to this program.
Their command of the subject is complemented by the effectiveness of the methodological design used in this Advanced master’s degree. Developed by a multidisciplinary team of e-learning experts, it integrates the latest advances in educational technology. In this way, students will be able to study with a range of comfortable and versatile multimedia tools that will give them the operability needed throughout the program.
The design of this program is based on Problem-Based Learning, an approach that views learning as a highly practical process. To achieve this remotely, we will use telepractice. With the help of an innovative, interactive video system and Learning from an Expert, students will be able to acquire the knowledge as if they were dealing with the case in real time. A concept that will allow students to integrate and memorize what they have learnt in a more realistic and permanent way.
TECH offers you the opportunity to take an in-depth and complete look into the strategies and approaches used in Veterinary Cardiology "

A program created for professionals who aspire to excellence, and that will enable you to easily and effectively acquire new skills and strategies"
Why study at TECH?
TECH is the world’s largest online university. With an impressive catalog of more than 14,000 university programs available in 11 languages, it is positioned as a leader in employability, with a 99% job placement rate. In addition, it relies on an enormous faculty of more than 6,000 professors of the highest international renown.

Study at the world's largest online university and guarantee your professional success. The future starts at TECH”
The world’s best online university according to FORBES
The prestigious Forbes magazine, specialized in business and finance, has highlighted TECH as “the world's best online university” This is what they have recently stated in an article in their digital edition in which they echo the success story of this institution, “thanks to the academic offer it provides, the selection of its teaching staff, and an innovative learning method aimed at educating the professionals of the future”
A revolutionary study method, a cutting-edge faculty and a practical focus: the key to TECH's success.
The most complete study plans on the university scene
TECH offers the most complete study plans on the university scene, with syllabuses that cover fundamental concepts and, at the same time, the main scientific advances in their specific scientific areas. In addition, these programs are continuously being updated to guarantee students the academic vanguard and the most in-demand professional skills. In this way, the university's qualifications provide its graduates with a significant advantage to propel their careers to success.
TECH offers the most comprehensive and intensive study plans on the current university scene.
A world-class teaching staff
TECH's teaching staff is made up of more than 6,000 professors with the highest international recognition. Professors, researchers and top executives of multinational companies, including Isaiah Covington, performance coach of the Boston Celtics; Magda Romanska, principal investigator at Harvard MetaLAB; Ignacio Wistumba, chairman of the department of translational molecular pathology at MD Anderson Cancer Center; and D.W. Pine, creative director of TIME magazine, among others.
Internationally renowned experts, specialized in different branches of Health, Technology, Communication and Business, form part of the TECH faculty.
A unique learning method
TECH is the first university to use Relearning in all its programs. It is the best online learning methodology, accredited with international teaching quality certifications, provided by prestigious educational agencies. In addition, this disruptive educational model is complemented with the “Case Method”, thereby setting up a unique online teaching strategy. Innovative teaching resources are also implemented, including detailed videos, infographics and interactive summaries.
TECH combines Relearning and the Case Method in all its university programs to guarantee excellent theoretical and practical learning, studying whenever and wherever you want.
The world's largest online university
TECH is the world’s largest online university. We are the largest educational institution, with the best and widest online educational catalog, one hundred percent online and covering the vast majority of areas of knowledge. We offer a large selection of our own degrees and accredited online undergraduate and postgraduate degrees. In total, more than 14,000 university degrees, in eleven different languages, make us the largest educational largest in the world.
TECH has the world's most extensive catalog of academic and official programs, available in more than 11 languages.
Google Premier Partner
The American technology giant has awarded TECH the Google Google Premier Partner badge. This award, which is only available to 3% of the world's companies, highlights the efficient, flexible and tailored experience that this university provides to students. The recognition as a Google Premier Partner not only accredits the maximum rigor, performance and investment in TECH's digital infrastructures, but also places this university as one of the world's leading technology companies.
Google has positioned TECH in the top 3% of the world's most important technology companies by awarding it its Google Premier Partner badge.
The official online university of the NBA
TECH is the official online university of the NBA. Thanks to our agreement with the biggest league in basketball, we offer our students exclusive university programs, as well as a wide variety of educational resources focused on the business of the league and other areas of the sports industry. Each program is made up of a uniquely designed syllabus and features exceptional guest hosts: professionals with a distinguished sports background who will offer their expertise on the most relevant topics.
TECH has been selected by the NBA, the world's top basketball league, as its official online university.
The top-rated university by its students
Students have positioned TECH as the world's top-rated university on the main review websites, with a highest rating of 4.9 out of 5, obtained from more than 1,000 reviews. These results consolidate TECH as the benchmark university institution at an international level, reflecting the excellence and positive impact of its educational model.” reflecting the excellence and positive impact of its educational model.”
TECH is the world’s top-rated university by its students.
Leaders in employability
TECH has managed to become the leading university in employability. 99% of its students obtain jobs in the academic field they have studied, within one year of completing any of the university's programs. A similar number achieve immediate career enhancement. All this thanks to a study methodology that bases its effectiveness on the acquisition of practical skills, which are absolutely necessary for professional development.
99% of TECH graduates find a job within a year of completing their studies.
Advanced Master's Degree in Veterinary Cardiology
.
Veterinary cardiology has undergone great advances in recent years, which has favored the emergence of new techniques for the approach of cardiac pathologies associated with animals. For this reason, it is important that professionals are updated in the latest methods of diagnosis, treatment and intervention of any type of cardiovascular alteration in order to be able to offer a service of greater guarantee and safety to patients. At TECH Global University we have developed the Advanced Master's Degree in Veterinary Cardiology, a specialization program that will help you prepare to take on the challenges of this discipline by using the most effective tools in your daily practice. If you want to acquire a higher level of knowledge and stand out as an expert in the area, don't wait any longer, get certified now!
Specialize in the largest Veterinary Faculty
.
With our Advanced Master's Degree you will have at hand a postgraduate degree of the highest academic level, supported by the latest methods and technologies for specialization in veterinary cardiology. You will study the cardiac and vascular physiology of different animal species; you will examine the pathophysiological mechanisms associated with this organ, and determine the mechanisms of intervention required in treatment, including the use of drugs or surgical techniques. You will establish appropriate methodologies for cardiovascular exploration, both in large and small species, and apply diagnostic protocols in order to detect the presence of any cardiac insufficiency and systemic diseases that may affect the cardiovascular system. At the largest veterinary school, you have a unique, innovative and effective opportunity to further your career growth.







