University certificate
The world's largest faculty of nursing”
Introduction to the Program
Update yourself in the latest methods of care for patients with Infectious Diseases by combining online learning with a practical stay in a prestigious clinical center"
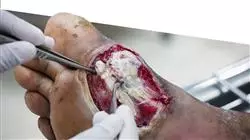
The care of infectious diseases in the field of hospital emergencies requires a high level of training by nurses, professionals who are increasingly demanded to be better prepared in relation to new infectious diseases that have increased their prevalence in recent years.
For this reason, TECH has designed this Hybrid Master's Degree that includes the classic aspects in the management of infectious pathology by apparatus or organs, taking into account the updates that may have occurred up to the time of the design of this program. But it has also incorporated new and essential items for a correct management of infectious diseases in the current scenario of globalization of health.
The content of this Hybrid Master's Degree is focused on the detailed updating of nursing professionals working in the emergency department attending patients with infectious diseases, whose functions require high levels of qualification, but also on the initiation of their activity as professionals in the field of research. Only with an adequate, focused and specialized refresher program can the knowledge and skills necessary to respond to the needs of these patients be acquired and maintained.
The aim is to respond to the growing need posed by the new challenges of a changing and increasingly demanding society, in order to raise awareness of the importance of incorporating new values, new work systems and new areas of action in this profession. Therefore, it is essential for the nursing professional to be able to respond adequately to people affected by an infectious disease, through adequate training for which they have to overcome personally and professionally.
Faced with this scenario, TECH presents this program that will allow the nurses to catch up with the most updated theory of the moment. In addition, they will be able to work with real patients and in a hospital setting with state-of-the-art resources, which will develop their maximum potential and growth in the area of infectious diseases. Thus, you will approach patients with infectious pathologies from the hand of the best specialists, using the latest techniques based on scientific evidence. All this, throughout 3 weeks of intensive practical stay in 8 consecutive hours days.
In addition to studying in online format, you will perform clinical practices in the emergency department with the highest standards of quality and technological level in an elite hospital center"
This Hybrid Master's Degree in Infectious Diseases in the Emergency Department for Nursing contains the most complete and up-to-date scientific program on the market. Its most outstanding features are:
- Development of more than 100 clinical cases presented by nursing professionals with expertise in Infectious Diseases
- The graphic, schematic, and practical contents with which they are created, provide scientific and practical information on the disciplines that are essential for professional practice
- Comprehensive systematized action plans for the main pathologies in the emergency department
- An algorithm-based interactive learning system for decision-making in the clinical situations presented throughout the course
- Practical clinical guides on approaching different pathologies
- Activities oriented to Infectious Diseases Nursing Specialists
- All of this will be complemented by theoretical lessons, questions to the expert, debate forums on controversial topics, and individual reflection assignments
- Content that is accessible from any fixed or portable device with an Internet connection
- In addition, you will be able to carry out a clinical internship in one of the best hospitals in the world
This Hybrid Master's Degree will allow you to incorporate into your daily work the protocols of Nursing action in patients with Infectious Diseases in the Emergency Department"
This Master's program, which has a professionalizing nature and a blended learning modality, is aimed at updating nursing professionals who perform their duties in the Emergency Department, and who require a high level of qualification. The content is based on the latest scientific evidence and is organized in a didactic way to integrate theoretical knowledge into nursing practice. The theoretical-practical elements allow professionals to update their knowledge and help them to make the right decisions in patient care.
Thanks to their multimedia content developed with the latest educational technology, they will allow the nursing professional to obtain situated and contextual learning, i.e., a simulated environment that will provide immersive learning programmed to train in real situations. This program is designed around Problem-Based Learning, whereby the professional must try to solve the different professional practice situations that arise throughout the program. For this purpose, the students will be assisted by an innovative interactive video system created by renowned experts.
Study from real clinical cases and interactive activities and apply what you learn in a 3-week intensive, face-to-face internship"
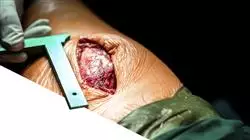
At TECH you will find a unique opportunity to improve your skills in the management of infectious diseases and provide more personalized care to your patients"
Syllabus
This Hybrid Master's Degree has the most complete and advanced syllabus in this area. In addition, the program is developed with a cutting-edge study methodology, known as Relearning, which allows nurses to combine their personal life with their studies. This learning system has been designed to take advantage of every minute invested in the TECH programs, making it perfect for working professionals who are short on time.

Enroll and access the most comprehensive syllabus in Infectious Diseases in the Emergency Department for Nursing. Don't wait any longer and take advantage of this opportunity"
Module 1. Up-to-date Information on Infectious Diseases
1.1. Principles of Infection
1.1.1. Virulence Factors and Toxins
1.1.2. Defensive Mechanisms of the Host
1.2. Main Human Pathogens in our Environment
1.2.1. Current Epidemiology of the Infection
1.2.2. Data on a Worldwide Level
1.2.3. Data in our Environment
1.2.4. Microbial Resistance
1.3. Current Scenarios of Infection in the Emergency Department
1.3.1. Elderly Patients
1.3.2. Oncology Patients
1.3.3. Chronic Renal Patients on Dialysis
1.3.4. Transplant Recipient
1.3.5. HIV Infection
1.3.6. Travelers and Immigrants
1.4. Etiopathogenic Profiles of Infection
1.4.1. Bacterial Infections
1.4.2. Viral Infections
1.4.3. Fungal Infections
1.4.4. Microbacterial Infections
1.4.5. Parasitic Infections
Module 2. The Microbiology Laboratory in the Emergency Department
2.1. Process of Sample Collection
2.1.1. General Considerations for Taking, Conserving and Transporting the Samples for Microbiological Study
2.1.2. Material for Sample Collection
2.2. Management of Samples in the Laboratory
2.2.1. Receiving Samples
2.2.2. Processing
2.2.3. Methods and Techniques used for Microbiological Diagnosis According to the Main Infectious Syndromes
2.3. Techniques Available for Emergency Diagnoses
2.3.1. Bacteria
2.3.2. Virus
2.3.3. Fungi
2.3.4. Mycobacteria
2.3.5. Parasites
2.4. Interpretation of Preliminary Results
2.4.1. Interpreatation of Microbiological Diagnostic Tests
2.5. Procedures in Hospitals Without On-call Microbiologists
2.5.1. Disadvantages of Not Having an On-call Microbiologist
2.5.2. Advantages of Having an On-call Microbiologist
2.5.3. On-call Care without a Microbiologist
Module 3. Public Health and Infectious Disease in the Emergency Department
3.1. Emergency Department Personnel
3.1.1. Initial Assessment
3.1.2. Vaccines
3.1.3. Action Protocols in Cases of Specific Exposure
3.2. Established Protocols of Isolation
3.2.1. Types of Transmission and Methods of Isolation
3.2.2. Special Situations
3.3. Notifiable Diseases and Urgent Declaration to Public Health
3.3.1. Concept of Notifiable Diseases
3.3.2. Surveillance of Notifiable Diseases
3.4. Special Situations
3.4.1. Annual Flu
3.4.2. Epidemiological Outbreaks
3.4.3. Imported Pathology Possibility of Pathology with High Contagious Capacity
3.5. Updates Epidemiological Outbreaks
3.5.1. Seasonal Epidemiological Parameters in the Most Common Infections in the Community
3.5.2. Epidemic Outbreak and Types of Source
3.6. Post-exposure Prophylaxis that is Initiated in the Emergency Department
3.6.1. Bacterial Meningitis
3.6.2. HIV Infection
3.6.3. Sexual Assault
3.6.4. Rabies
Module 4. Systemic Febrile Syndrome. Antimicrobials:
4.1. Biomarkers in Sepsis
4.1.1. Lactate
4.1.2. Procalcitonin
4.1.3. Proadrenomedulin
4.1.4. Combinations
4.2. Initial Focus in Acute Fever Syndrome
4.2.1. Initial Management of a Patient with a Fever in the Emergency Department
4.2.2. Treatment
4.2.3. Special Categories
4.2.4. Fever of Unknown Origin
4.2.5. Attitude and Destiny of the Patient
4.3. Bacteremia, Sepsis and Septic Shock
4.3.1. Definitions According to Consensus Conferences
4.3.2. How to Identify a Patient with Sepsis
4.3.3. Controversies and Limitations of the New Definitions
4.3.4. Managing Sepsis
4.4. Antimicrobials:
4.4.1. Concept: What is a Microbial?
4.4.2. Antibacterials
4.4.3. Pregnancy and Breastfeeding
4.4.4. Antifungal
Module 5. Emergency Diagnostic and Therapeutic Management of Fever in Special Situations
5.1. Fever in Emergencies
5.1.1. General Concepts
5.1.2. Action Protocol
5.1.3. Patient Orientation
5.2. Fever in an Elderly Patient
5.2.1. General Concepts
5.2.2. Characteristics of the Specific Clinical Framework
5.2.3. Points to Remember
5.3. Fever in a Hemodialysis Patient
5.3.1. Infections Related to Vascular Access in Hemodialysis
5.3.2. Other Considerations in the Infectious Pathology of a Patient on Dialysis
5.4. Fever in the Patient with Intravascular Catheters
5.4.1. Clinical Manifestations
5.4.2. Etiology
5.4.3. Diagnosis
5.4.4. Treatment
5.4.5. Prevention
5.5. Patient with HIV Infection
5.5.1. Pulmonary Syndromes
5.5.2. Neurological syndromes
5.5.3. Other Fever Syndromes
5.5.4. Immune Reconstitution Syndrome
5.6. Patient with Iatrogenic Immunosuppression
5.6.1. Etiology
5.6.2. Diagnostic Approach
5.6.3. Treatment
5.7. Patient with Onco-hematologic Pathology
5.7.1. Diagnosis and Therapeutic Management of an Onco-hematologic Patient with a Fever
5.8. Transplant Recipient of a Solid Organ
5.8.1. Infections in the First Month Post-Transplant
5.8.2. Infections Between the First and Sixth Month Post-Transplant
5.8.3. Infections After the Sixth Month Post-Transplant
5.8.4. Diagnostic Strategy
5.8.5. Empirical Treatment
5.9. Patient who has Recently Undergone Surgery
5.9.1. Infection of Surgical Wounds Current Management
5.9.2. Other Infections in a Patient who has Recently Undergone Surgery
5.10. Pregnant Patient
5.10.1. Special Characteristics of a Pregnant Woman
5.10.2. Diagnostic Orientation in the Emergency Department
5.10.3. Treatment and Management in Special Situations
5.10.4. Indications of Admission for Observation and Inpatient Treatment
Module 6. Infections of Organs and Apparatus (I): ORL, Head and Neck, Ophthalmological
6.1. Pharyngotonsillitis
6.1.1. General Concept and Classification
6.2. Oral Cavity, Head and Neck Infections
6.2.1. Plaque Gingivitis
6.2.2. GUNA
6.2.3. Oral TB
6.2.4. Oral Syphilis
6.2.5. Oral Mycosis
6.2.6. Viral Infections
6.3. Otitis Externa, Media and Mastoiditis
6.3.1. Diffuse Otitis Externa and Circumscribed Otitis Externa (boils)
6.3.2. Otomycosis
6.3.3. Malignant Otitis Externa
6.3.4. Optic Herpes
6.3.5. Bullous Myringitis
6.3.6. Acute Otitis Media
6.3.7. Mastoiditis
6.4. Sinusitis
6.4.1. Pathophysiology
6.4.2. Classification According to Etiology and Severity
6.4.3. Symptoms
6.4.4. Diagnosis
6.4.5. Complementary Tests
6.4.6. Treatment
6.4.7. Complications
6.5. Peritonsillar, Parapharyngeal and Retropharyngeal Abscesses
6.5.1. Peritonsillar Abscess
6.5.2. Parapharyngeal Space Infection
6.5.3. Retropharyngeal Space Infection
6.6. Dental Infections
6.6.1. Etiological Factors
6.6.2. Etiopathogenesis
6.6.3. Clinical Symptoms
6.6.4. Diagnosis
6.6.5. Treatment
6.7. Mucositis and Stomatitis
6.7.1. Trauma Lesions
6.7.2. Lesions Caused by Chemical Agents
6.7.3. Allergic Stomatitis
6.7.4. Oral Drug Ulcers by Unknown Mechanisms
6.7.5. Gingival Alterations Caused by Drugs
6.7.6. Facial Reaction to Esthetic Fillers
6.7.7. Oral Lesions Caused by Cocaine
6.7.8. Oral Mucosal Dyschromias due to Exogenous Pigmentation
6.7.9. Injuries Caused by Physical Agents
6.7.10. Recurrent Aphthous Stomatitis
6.7.11. Erythema Multiform
6.8. Infection of Salivary Glands
6.8.1. General Aspects. Anamnesis and Examination Complementary Methods
6.8.2. Viral Infection
6.8.3. Bacterial Infections
6.8.4. Sialodochitis or Obstructive Pathology of the Salivary Glands
6.9. Acute Laryngitis and Epiglottitis
6.9.1. Acute Laryngitis
6.9.2. Tuberculous Laryngitis
6.9.3. Epiglottitis
6.10. Conjunctivitis and Keratitis
6.10.1. Infectious Conjunctivitis
6.10.2. Concept and General Considerations
6.10.3. Bacterial Conjunctivitis
6.10.4. Viral Conjunctivitis
6.10.5. Mycotic or Parasitic Conjunctivitis
6.10.6. Infectious Keratitis
6.10.7. Concept and General Considerations
6.10.8. Bacterial Keratitis
6.10.9. Viral Keratitis
6.10.10. Mycotic Keratitis
6.10.11. Acanthamoeba Keratitis
6.11. Uveitis, Endophthalmitis, and Retinitis
6.11.1. Uveitis: Concepts and Classification
6.11.2. Parasitic Uveitis
6.11.3. Viral Uveitis
6.11.4. Fungal Uveitis
6.11.5. Bacterial Uveitis
6.12. Periocular Infections
6.12.1. Stye
6.12.2. Chronic Canaliculitis
6.12.3. Acute Dacryocystitis
6.12.4. Preseptal Cellulitis
6.12.5. Postseptal (orbital) Celulitis
6.12.6. Acute Dacryoadenitis: Inflammation of the Lacrimal Gland
6.12.7. Viral Infections
6.12.8. Other Periocular Infections
Module 7. Infections of Organs and Apparatus (II): Skin, Soft and Osteoarticular
7.1. Cellulitis and Superficial Infections
7.1.1. Clinical Symptoms
7.1.2. Diagnosis
7.1.3. Treatment
7.2. Deep Infections
7.2.1. Necrotizing Fasciitis
7.2.2. Fournier's Gangrene
7.2.3. Infectious Myositis
7.3. Diabetic Foot
7.3.1. Etiopathogenesis
7.3.2. Clinical Symptoms
7.3.3. Staging Classification of Ulcers of Infected Diabetic Foot
7.3.4. Etiology
7.3.5. Diagnosis. Complementary Evaluations
7.3.6. Treatment
7.4. Pressure Ulcers
7.4.1. Etiopathogenesis
7.4.2. Risk Factors
7.4.3. Clinical Assessment
7.4.4. Complications
7.4.5. Treatment
7.4.6. Infection of Pressure Lesions
7.5. Septic Arthritis
7.5.1. Epidemiology
7.5.2. Pathophysiology
7.5.3. Etiology
7.5.4. Clinical Symptoms
7.5.5. Diagnosis
7.5.6. Differential Diagnosis
7.5.7. Treatment
7.5.8. Prognosis
7.6. Osteomyelitis
7.6.1. Classification
7.6.2. Etiology and Clinical Characteristics
7.6.3. Diagnosis
7.6.4. Treatment
7.7. Spondylodiscitis
7.7.1. Etiopathogenesis and Microbiology
7.7.2. Clinical Manifestations
7.7.3. Diagnosis
7.7.4. Treatment
7.7.5. Prognosis
7.8. Infection of Joint Prostheses and Osteosynthesis Material
7.8.1. Etiopathogenesis
7.8.2. Diagnostic Approximation
7.8.3. Treatment Management
Module 8. Infections of Organs and Apparatus (III): Lower Airway, Intra-abdominal
8.1. Acute Bronchitis
8.1.1. Definition
8.1.2. Clinical Manifestations
8.1.3. Diagnosis
8.1.4. Treatment
8.2. Acute Chronic Obstructive Pulmonary Disease (COPD)
8.2.1. Definition
8.2.2. Diagnosis
8.2.3. Treatment
8.2.4. Attitude to Clinical Failure
8.2.5. Key Concepts
8.3. Community-Acquired Pneumonia (CAP)
8.3.1. Concept
8.3.2. Pathophysiology
8.3.3. Epidemiology
8.3.4. Etiology
8.3.5. Clinical Manifestations
8.3.6. Diagnostic Attitude
8.3.7. Antibiotic Treatment
8.4. Healthcare-Associated Pneumonia (HAP)
8.4.1. Concept
8.4.2. Healthcare-Associated Pneumonia Versus Community-Acquired Pneumonia due to Resistant Pathogens (CAP-PR)
8.4.3. Etiology
8.4.4. Microbiological Diagnosis
8.4.5. Empirical Treatment
8.4.6. Prognosis
8.5. Pneumonic Pleural Effusion and Empyema
8.5.1. Clinical Symptoms
8.5.2. Staging
8.5.3. Imaging Tests
8.5.4. Laboratory Studies: Pleural Fluid Analysis
8.5.5. Pathophysiology Staging
8.5.6. Bacteriology
8.5.7. Prognosis
8.5.8. Treatment
8.6. Pulmonary Abscess
8.6.1. Definition
8.6.2. Etiology
8.6.3. Pathophysiology
8.6.4. Clinical Manifestations
8.6.5. Diagnosis
8.6.6. Treatment
8.7. Pulmonary Tuberculosis
8.7.1. Etiology
8.7.2. Clinical Manifestations
8.7.3. Diagnosis
8.7.4. Treatment
8.8. Gastroenteritis
8.8.1. Etiology
8.8.2. Clinical Manifestations and Physical Examination
8.8.3. Laboratory Data and Imaging Tests
8.8.4. Diagnosis
8.8.5. Treatment
8.9. Liver and Biliary Tract Infections
8.9.1. Bacterial Infections which Affect the Liver
8.9.2. Viral Infections which Affect the Liver
8.9.3. Parasitic Infections which Affect the Liver
8.9.4. Fungal Infections which Affect the Liver
8.10. Cholecystitis and Cholangitis
8.10.1. Acute Cholecystitis
8.10.2. Acute Cholangitis
8.11. Liver Abscesses
8.11.1. Concept and General Characteristics
8.11.2. Classification and Etiopathogenesis
8.11.3. Pyogenic Hepatic Abscesses
8.11.4. Amoebic Liver Abscesses
8.12. Acute Hepatitis
8.12.1. Definition
8.12.2. Etiology
8.12.3. Clinical Manifestations and Physical Examination
8.12.4. Laboratory Data
8.12.5. Diagnosis
8.12.6. Severe Acute Hepatitis
8.12.7. Severe Acute Liver Failure
8.12.8. Treatment
8.13. Pancreatitis
8.13.1. Etiology
8.13.2. Diagnosis
8.13.3. Classification
8.13.4. Severity Prediciton and Prognostic
8.13.5. Treatment
8.13.6. Infectious Complications
8.14. Appendicitis
8.14.1. Epidemiology
8.14.2. Etiopathogenesis
8.14.3. Microbiology
8.14.4. Diagnosis
8.14.5. Differential Diagnosis
8.14.6. Treatment
8.14.7. Preoperative Antibiotic Prophylaxis
8.14.8. Postoperative Antibiotic Treatment
8.14.9. Post-surgery Complications
8.15. Diverticulitis and Perirectal Abscess
8.15.1. Definition of Diverticulitis
8.15.2. Pathogenesis
8.15.3. Risk Factors
8.15.4. Diverticulitis Diagnosis
8.15.5. Diverticulitis Classification
8.15.6. Treatment for Diverticulitis
8.15.7. Perirectal Absess
8.16. Typhlitis
8.16.1. Epidemiology
8.16.2. Etiology
8.16.3. Pathogenesis
8.16.4. Clinical Manifestations
8.16.5. Diagnosis
8.16.6. Differential Diagnosis
8.16.7. Treatment
8.17. Peritonitis
8.17.1. Classification
8.17.2. Pathogenesis
8.17.3. Diagnosis
8.17.4. Assess the Severity of the Infection
8.17.5. Treatment
8.18. Spontaneous Bacterial Peritonitis
8.18.1. Concept
8.18.2. Epidemiology
8.18.3. Pathogenesis
8.18.4. Clinical Manifestations
8.18.5. Diagnosis
8.18.6. Prognosis
8.18.7. Treatment
8.18.8. Prophylaxis
8.19. Secondary Peritonitis
8.19.1. Definition and Classification
8.19.2. Microbiology
8.19.3. Evaluation of Severity
8.19.4. General Principles for the Management
8.20. Intraperitoneal Absess
8.20.1. Definition
8.20.2. Epidemiology
8.20.3. Etiology and Pathophysiology
8.20.4. Diagnosis
8.20.5. Treatment
Module 9. Infections of Organs and Apparatus (IV): Cardiovascular, CNS
9.1. Infectious Endocarditis
9.1.1. Epidemiology
9.1.2. Etiology
9.1.3. Clinical Symptoms
9.1.4. Diagnosis
9.1.5. Treatment
9.1.6. Prevention
9.2. Infection of Intravascular Devices
9.2.1. Infections Associated with Intravascular Catheter
9.2.2. Infections Related to Implantable Electronic Cardiovascular Implantable Cardiovascular Devices
9.3. Acute Pericarditis
9.3.1. Definition
9.3.2. Incessant and Chronic Pericarditis
9.3.3. Recurrent Pericarditis
9.3.4. Myopericarditis
9.4. Mediastinitis
9.4.1. Acute Mediastinitis
9.4.2. Sclerosing Mediastinitis
9.5. Meningitis
9.5.1. Epidemiology and Etiopathogenesis
9.5.2. Diagnosis of Meningitis: Clinical and Laboratory
9.5.3. Antimicrobial Treatment
9.6. Encephalitis
9.6.1. Epidemiology and Etiopathogenesis
9.6.2. Diagnosis of Encephalitis: Clinical and Complementary Evaluations
9.6.3. Antimicrobial Treatment
9.7. Myelitis
9.7.1. Epidemiology and Etiopathogenesis
9.7.2. Clinical Symptoms
9.7.3. Diagnosis
9.7.4. Treatment
9.8. Cerebral Absess
9.8.1. Etiopathogenesis
9.8.2. Clinical Manifestations and Diagnosis
9.8.3. Treatment
9.9. Subdural Empyema, Epidural Abscess and Intracranial Thrombophlebitis
9.9.1. Subdural Empyema: Etiopathogenesis, Clinical Manifestations, Diagnosis and Treatment
9.9.2. Epidural Abscess: Etiopathogenesis, Clinical Manifestations, Diagnosis and Treatment
9.9.3. Septic Thrombophlebitis: Etiopathogenesis, Clinical Manifestations, Diagnosis and Treatment
9.10. CSF Shunt Infections
9.10.1. Etiopathogenesis
9.10.2. Clinical Manifestations
9.10.3. Diagnosis
9.10.4. Treatment
Module 10. Infections of Urinary Tract, Genitals and Sexual Transmission
10.1. Cystitis
10.1.1. Symptoms
10.1.2. Etiology
10.1.3. Diagnosis
10.1.4. Differential Diagnosis
10.1.5. Treatment
10.2. Asymptomatic Bacteriuria
10.2.1. Epidemiology
10.2.2. Pathophysiology
10.2.3. Assessment and Treatment
10.3. UTI in Patients with Bladder Catheterization
10.3.1. Etiology
10.3.2. Clinical Manifestations
10.3.3. Diagnosis
10.3.4. Prevention
10.3.5. Treatment
10.4. Prostatitis
10.4.1. Etiopathogenesis
10.4.2. Diagnosis
10.4.3. Clinical Symptoms
10.4.4. Treatment
10.4.5. Complications
10.5. Chronic Nonbacterial or Chronic Idiopathic Prostatitis or Chronic Pelvic Pain Syndrome
10.5.1. Pyelonephritis
10.5.1.1. Etiology
10.5.1.2. Clinical Manifestations
10.5.1.3. Complementary Tests
10.5.1.4. Treatment
10.5.1.5. Admission Criteria
10.5.2. Perinephritic Abscess
10.5.2.1. Pathophysiology
10.5.2.2. Clinical Symptoms
10.5.2.3. Etiology
10.5.2.4. Diagnosis
10.5.2.5. Assessment and Treatment
10.5.3. Infections which Cause Skin and Genital Mucosal Lesions
10.5.3.1. Bacterial Infections
10.5.3.2. Fungal Infections
10.5.3.3. Viral Infections
Module 11. Infectious Diseases in Pediatric Patients in the Emergency Department
11.1. Fever Without Focus
11.1.1. Child With a Fever Without Focus and Poor Appearance
11.1.2. Fever Without Focus and Good General Appearance
11.1.3. Children from 3-36 Months Old With a Fever Without Focus and Good General Appearance
11.1.4. Breastfeeding Infant less than 3 Months Old With a Fever Without Focus and Good General Appearance
11.2. Sepsis and Septic Shock
11.2.1. Concept
11.2.2. Current Definition of Shock and Septic Shock
11.2.3. Etiology and Epidemiology
11.2.4. Pathophysiology
11.2.5. Risk Factors
11.2.6. Differential Diagnosis
11.2.7. Clinical Symptoms
11.2.8. Complementary Tests
11.2.9. Treatment
11.3. Fever in a Traveling Child
11.3.1. Medical History
11.3.2. Physical Examination
11.3.3. Complementary Tests
11.3.4. Treatment
11.3.5. Malaria
11.3.6. Dengue
11.4. Exanthem
11.4.1. Etiology
11.4.2. Diagnosis
11.4.3. Differential Diagnosis
11.5. Skin and Soft Tissue Infections
11.5.1. Etiopathogenesis
11.5.2. Diagnosis
11.5.3. Main Clinical Framework
11.5.4. Treatment
11.5.5. Community-acquired Methicillin-Resistant S. Aureus
11.6. Cervical Adenitis
11.6.1. Etiology
11.6.2. Clinical Assessment
11.6.3. Diagnosis and Treatment
11.6.4. Differential Diagnosis
11.7. Osteoarticular Infections: Acute Osteomyelitis and Septic Arthritis
11.7.1. Epidemiology
11.7.2. Etiopathogenesis
11.7.3. Clinical Symptoms
11.7.4. Diagnosis
11.7.5. Differential Diagnosis
11.7.6. Treatment
11.8. Pharyngotonsillitis and Its Complications
11.8.1. Concept
11.8.2. Epidemiology and Etiology
11.8.3. Clinical Symptoms
11.8.4. Diagnosis
11.8.5. Treatment
11.9. Otitis Media and External Sinusitis
11.9.1. Concept of Otitis Media and External
11.9.1.1. Epidemiology and Etiology
11.9.1.2. Clinical Symptoms
11.9.1.3. Complications
11.9.1.4. Diagnosis
11.9.1.5. Treatment
11.9.2. Concept of Acute Sinusitis
11.9.2.1. Epidemiology and Etiology
11.9.2.2. Clinical Symptoms
11.9.2.3. Diagnosis
11.9.2.4. Treatment
11.10. Acute Mumps
11.10.1. Epidemic Mumps
11.10.2. Vaccines
11.10.3. Prevention of Epidemic Outbreaks
11.11. Laryngitis and Epiglottitis
11.11.1. Concept
11.11.2. Epidemiology and Etiology
11.11.3. Clinical Symptoms
11.11.4. Diagnosis
11.11.5. Treatment
11.11.6. Admission Criteria
11.12. Syndrome Pertusoids
11.12.1. Concept
11.12.2. Epidemiology and Etiology
11.12.3. Clinical Symptoms
11.12.4. Complications
11.12.5. Diagnosis
11.12.6. Treatment
11.12.7. Prevention
11.13. Bronchiolitis and Recurrent Wheezing Episodes
11.13.1. Acute Bronchiolitis
11.13.2. Recurrent Wheezing
11.14. Pneumonia and Complications
11.14.1. Epidemiology
11.14.2. Etiology
11.14.3. Clinical Characteristics
11.14.4. Diagnosis
11.14.5. Treatment
11.14.6. Prevention
11.14.7. Complications
11.15. Tuberculosis
11.15.1. Manifestations
11.15.2. Diagnosis
11.15.3. Treatment
11.16. Acute Gastroenteritis
11.16.1. Etiopathogenesis
11.16.2. Clinical Symptoms
11.16.3. Diagnosis
11.16.4. Treatment
11.17. Viral Hepatitis
11.17.1. Evaluation and Initial Management of Hepatitis in the Emergency Department
11.17.2. Classic Viral Hepatitis
11.18. Appendicitis (Need for Antibiotic or Not) and Perirectal Absesses
11.18.1. Acute Appendicitis
11.18.2. Perirectal Absess
11.19. Urinary Infection
11.19.1. Definition
11.19.2. Etiopathogenesis
11.19.3. Clinical. When to suspect a urinary tract infection in the pediatric age?
11.19.4. Diagnosis
11.19.5. Management
11.20. CNS Infections in Pediatrics: Acute Meningitis
11.20.1. Etiology
11.20.2. Clinical Symptoms
11.20.3. Diagnosis
11.20.4. Treatment
11.20.5. Chemoprophylaxis
11.20.6. Complications and Prognosis
11.21. Endocarditis, Myocarditis and Pericarditis
11.21.1. Infectious Endocarditis
11.21.2. Myocarditis
11.21.3. Pericarditis
11.22. Treatment in Pediatric Infectious Diseases
11.22.1. Bacterial Infections in the Pediatric Emergency Department: Diagnosis and Antibiotic Treatment of Choice, Depending on the Resistance of the Pathogens Responsible for the Disease
11.22.2. Delayed Antibiotic Prescribing Strategy
11.22.3. When is the Association of Amoxicillin with Clavulanic Acid and Macrolides Indicated in Pediatrics?
11.22.4. Do I Also Have to be Careful with Topical Antibiotherapy to Avoid Bacterial Resistance?
Module 12. Imported Infectious Diseases in the Emergency Department
12.1. Introduction to Imported Pathology
12.1.1. Imported Pathology of Special Interest
12.1.1.1. Chagas Disease
12.1.1.2. Dengue
12.1.1.3. Chikungunya
12.1.1.4. Malaria
12.2. Globalization and Emerging Pathology
12.2.1. Emerging and Re-emerging Diseases
12.2.2. Main Causes of Emergency in Infectious Diseases
12.2.3. Transmission
12.2.4. Zoonotic
12.2.5. Future Previsions
12.3. Geography of Tropical Infectious Diseases
12.3.1. Subspecialties of Medical Geography
12.3.2. Relevance and Relationship to Tropical Diseases
12.3.3. Main Infectious Diseases According to Area
12.4. Epidemiology of Tropical Infectious Diseases in Travelers, Immigrants and VFRs
12.4.1. Importance
12.4.2. Epidemiological Characteristics of Immigrants
12.4.3. Epidemiological Characteristics of People Traveling to the Tropics
12.4.4. Epidemiological Characteristics of VFRs
12.4.5. Data on Imported Pathology in Spain
12.5. Anamnesis of a Traveler with Fever in the Emergency Department
12.5.1. Initial Approximation of a Traveler with Fever
12.5.2. Differential Diagnosis
12.5.3. Treatment of a Traveler with Fever
12.6. Fever After Staying in a Tropical and / or Subtropical Area
12.6.1. Importancce of Good Anamnesis
12.6.2. Investigation of Possible Vectors
12.6.3. Fever of Parasitic Origin
12.6.4. Fever of Viral Origin
12.6.5. Fever of Bacterial Origin
12.6.6. Other Causes of Fever
12.7. Imported Infectious Pathology Syndrome Classification
12.7.1. Fever and Cutaneous Lesion
12.7.2. Fever and Altered Level of Consciousness
12.7.3. Fever and Liver Problems
12.7.4. Fever and Respiratory Semiology
12.7.5. Fever and Digestive Semiology
12.8. Imported Tropical Infectious Diseases of Special Interest
12.8.1. Malaria
12.8.2. Arbovirus: Dengue, Zika, Chikungunya
12.8.3. MERS Coronavirus (MERS CoV)
12.8.4. Schistosomiasis
12.8.5. Invasive Enteritis (Salmonella, Shigella, E.coli, Campylobacter)
12.8.6. Hemorrhagic Fevers (Ebola, Lassa, Marburg, Yellow Fever, Crimean-Congo)
Module 13. Update on Coronavirus Infections
13.1. Discovery and Evolution of Coronaviruses
13.1.1. Discovery of Coronaviruses
13.1.2. Global Trends in Coronavirus Infections
13.2. Main Microbiological Characteristics and Members of the Coronavirus Family
13.2.1. General Microbiological Characteristics of Coronaviruses
13.2.2. Viral Genome
13.2.3. Principal Virulence Factors
13.3. Epidemiological Changes in Coronavirus Infections from its Discovery to the Present
13.3.1. Morbidity and Mortality of Coronavirus Infections from their Emergence to the Present
13.4. The Immune System and Coronavirus Infections
13.4.1. Immunological Mechanisms Involved in the Immune Response to Coronaviruses
13.4.2. Cytokine Storm in Coronavirus Infections and Immunopathology
13.4.3. Modulation of the Immune System in Coronavirus Infections
13.5. Pathogenesis and Pathophysiology of Coronavirus Infections
13.5.1. Pathophysiological and Pathogenic Alterations in Coronavirus Infections
13.5.2. Clinical Implications of the Main Pathophysiological Alterations
13.6. Risk Groups and Transmission Mechanisms of Coronaviruses
13.6.1. Main Sociodemographic and Epidemiological Characteristics of Risk Groups Affected by Coronavirus
13.6.2. Coronavirus Mechanisms of Transmission
13.7. Natural History of Coronavirus Infections
13.7.1. Stages of Coronavirus Infection
13.8. Latest Information on Microbiological Diagnosis of Coronavirus Infections
13.8.1. Sample Collection and Shipment
13.8.2. PCR and Sequencing
13.8.3. Serology Testing
13.8.4. Virus Isolation
13.9. Current Biosafety Measures in Microbiology Laboratories for Coronavirus Sample Handling
13.9.1. Biosafety Measures for Coronavirus Sample Handling
13.10. Up-to-Date Management of Coronavirus Infections
13.10.1. Prevention Measures
13.10.2. Symptomatic Treatment
13.10.3. Antiviral and Antimicrobial Treatment in Coronavirus Infections
13.10.4. Treatment of Severe Clinical Forms
13.11. Future Challenges in the Prevention, Diagnosis, and Treatment of Coronavirus
13.11.1. Global Challenges for the Development of Prevention, Diagnostic, and Treatment Strategies for Coronavirus Infections

Enroll now and advance in your field of work with a comprehensive program that will allow you to put into practice everything you have learned"
Hybrid Master's Degree in Infectious Diseases in the Emergency Department for Nursing
Are you passionate about the fascinating world of Infectious Diseases in the Emergency Department? Do you want to acquire the necessary knowledge to become an expert in this field of vital importance for public health? We have the answer you were looking for! The Hybrid Master's Degree in Infectious Diseases in the Emergency, offered by the prestigious School of Nursing at TECH Global University, is your gateway to a promising future. Imagine being able to study from the comfort of your home, in a virtual environment that adapts to your schedule, allowing you to reconcile your personal and professional life. Does this sound incredible? But that's not all! At the end of the theoretical sessions online, you will have the opportunity to interact directly with experts in the field, strengthening your clinical skills and putting into practice everything you have learned. Our teaching team is made up of highly qualified professionals, committed to providing you with a specialization of excellence. Their experience and expertise will guide you every step of the way, ensuring that you acquire the competencies necessary to meet the challenges of managing infectious diseases in the emergency setting.
They will help you develop the skills you need to meet the challenges of managing infectious diseases in the emergency setting.
They will guide you every step of the way, ensuring that you acquire the skills you need to meet the challenges of managing infectious diseases in the emergency setting.
They will guide you every step of the way.
Enroll today and take the first step towards professional success!
During the Hybrid Master's Degree, you will thoroughly explore the theoretical and practical aspects related to infectious diseases in emergency settings. You will learn to identify, diagnose and effectively treat a wide variety of infectious pathologies, acquiring the skills necessary to safeguard the health of patients and prevent the spread of disease. Upon completion of the program, you will obtain a certificate endorsed by TECH Global University, a prestigious document recognized in the field of health. This certificate will open the doors to a wide range of job opportunities, both in the public and private sectors. You will be able to work as a specialist in infectious diseases in hospitals, primary care centers, research institutions and international organizations. Don't miss this unique opportunity to develop your career and make a difference in the fight against infectious diseases in the emergency department. Enroll in the Hybrid Master's Degree in Infectious Diseases in the Emergency Department for Nursing at TECH Global University and prepare yourself for a challenging and successful future!







